Diabetes as a Global Epidemic: Prevention and Management Across Border
Reviewed by: Manipal Hospitals Global
Posted on Aug 28, 2025
6 Min Read

Synopsis
- Global Prevalence and Impact
- Causes and Risk Factors
- Regional Differences and Inequities
- Prevention Across Borders
- Management Challenges
- International Cooperation and Innovation
- Frequently Asked Questions
Global Prevalence and Impact
As of 2025, an estimated 589 million adults between the ages of 20 and 79—nearly one in nine—were living with diabetes in the world. More than 81% of those living with diabetes were in low- and middle-income countries with limited healthcare access.
Projected estimates suggest the number will jump significantly to an estimated 853 million adults by 2050—this is nearly one in eight—of which more than 40% remain undiagnosed. This marks a hidden epidemic and a pressing need for improved screening.
Not only is the overall number increasing, but the rate of growth is significant as well. The last 30 years has seen cases of diabetes quadruple—there were just over 200 million in 1990 to nearly 830 million in 2022. In 2024 alone, diabetes caused an estimated 3.4 million deaths that year and more than one trillion dollars in global health expenditures.
Causes and Risk Factors
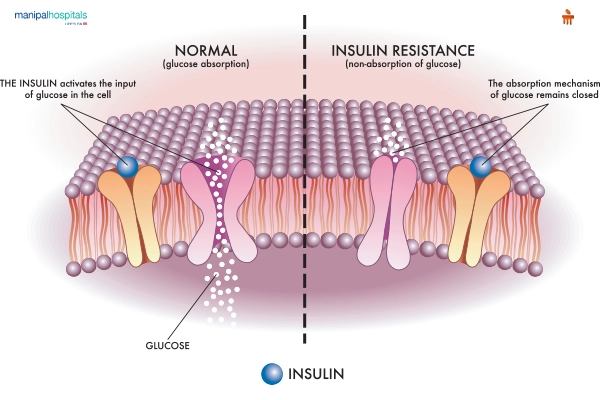
Over 90% of the people suffering from diabetes have type 2, which is the type most associated with socioeconomic and lifestyle factors. The rapid urbanization, aging population, declining physical activity levels, and increasing rates of overweight and obesity have all contributed to the rise of type 2 diabetes. Genetic and family history are also important factors. Even when rates are rising, many do not realize they have diabetes, which leads to a delay in treatment and increases the possibility of severe complications that could threaten their life.
Regional Differences and Inequities
In some areas, including South-East Asia and the Eastern Mediterranean, the prevalence rate of diabetes for adults without distinction as to type can be as high as 20%. In many low-and middle-income countries, public health systems often do not have sufficient primary care, and people with T2DM have little, if any, access to a diagnosis, education, or access to medications such as insulin to allow them access to diabetes-related glucose lowering medications to avoid long-term complications. Not surprisingly, fewer than 40% of residents in low- and middle-income countries access glucose lowering medications.
This contrasts significantly with high-income countries. Although diagnosis and long-term management rates remain high, high-income countries are seeing increases in the number of new diagnoses of T2DM. This increase follows the global trend to sedentary lifestyles and dietary changes. Additionally, vulnerable groups such as ethnic minorities and people whose socioeconomic status limits access to proper care and support are only increasing in number.
Prevention Across Borders
The consensus from science is clear: type 2 diabetes can be prevented or at least postponed in many at-risk individuals. High risk individual strategies include:
- Encouraging healthy eating (less processed and added sugar and unhealthy fats).
- Increasing safe opportunities for regular physical activity in schools, workplaces, and communities.
- Making it easier to limit unhealthy food and beverage advertisements and marketing.
- Addressing overweight and obesity and helping people achieve a healthy weight.
National and international frameworks, such as those promoted by the World Health Organization (WHO) and the International Diabetes Federation (IDF), guide countries in surveillance, health promotion, and policy responses. However, the reach and effectiveness of these programs often fall short in the face of underfunded health systems, social inequities, and political challenges.
Management Challenges
Effective management of diabetes—including both type 1 and type 2—relies heavily on robust health systems. Major challenges encountered, especially in resource-constrained settings, include:
- Lack of specialized medical personnel and supportive staff.
- Outdated or unclear clinical guidelines for diabetes care.
- Scarcity and high cost of essential medicines and supplies, including insulin.
- High out-of-pocket expenditures, with minimal health insurance coverage.
- Interruption of care during emergencies or disasters.
- Limited opportunities for continuing education of healthcare providers.
For patients, education and empowerment is essential. Individuals living with diabetes must have continual access to guidance regarding blood sugars, nutrition, exercise, and early identification of complications. Community-based programs and digital health methods are shining beacons of opportunity for providing ongoing diabetes care, especially patients who live in rural or marginalized communities.
International Cooperation and Innovation
Considering the shared aspects of the diabetes epidemic, international collaborations for research, knowledge exchange and capacity building continues to be important. The Global Diabetes Compact to which WHO is a signatory, and similar initiatives, help to harmonise data collection, provide guidance for resource allocation, and catalyse action for global health targets.
Innovations: Development of new prevention programs and medications, and digital technologies for monitoring and support beyond the traditional clinical context, need urgent attention. National policies should align with the global Sustainable Development Goals, which provides a momentous opportunity to act together in relation to diabetes and the wider burden of noncommunicable diseases.


Manipal Hospitals Global is dedicated to tackling diabetes as a global health challenge. Through exceptional expertise in Diabetes Care in India, advanced technology, and patient-centric care, Manipal Hospitals one of the Leading Diabetes Hospital places an emphasis on prevention, early detection and comprehensive management of diabetes and its complications across the continuum of diabetes care--while making sure that international patients never feel any breaks in care to provide seamless, comprehensive care.
With the nature of diabetes care being multidisciplinary with a personalized care plan, along with digital health solutions to bridge gaps to access of care, Manipal Hospitals helps to empower persons to take ownership of their health, and help obtain the best excellence in diabetes care possible, regardless of where you live.
Share this Article


Not sure what you’re looking for?
Not sure what you’re looking for?
Get in touch with our representatives for
help!
Get in touch with our
representatives for help!

