Planning Bariatric Surgery Overseas? Benefits, Risks, and Recovery Timeline
Reviewed by: Dr Sandeep Aggarwal
Posted on Jan 26, 2026
10 Min Read

In recent years, thousands of people have started exploring bariatric surgery overseas due to better access to expert surgeons, shorter waiting times, bundled care packages, and affordable hospital treatment plans. However, travelling for surgery also requires careful planning—because successful outcomes depend not only on the procedure, but also on pre-operative preparation, medical safety checks, nutrition planning, and proper follow-up after returning home.
This guide is created specifically for international patients to understand what bariatric surgery is, the benefits and risks, how to prepare for surgery abroad, and the recovery timeline you can realistically expect.
Synopsis
- What is Bariatric Surgery?
- Who is Eligible for Bariatric Surgery?
- Key Benefits of Bariatric Surgery
- Bariatric Surgery Options for International Patients
- Why Patients Choose Bariatric Surgery Overseas
- Bariatric Surgery Cost: What International Patients Should Know
- Risks of Bariatric Surgery (Realistic and Medically Accurate)
- Preparing for Bariatric Surgery Hospital Admission, Surgery & Discharge Flow
- Bariatric Surgery Recovery Timeline (Week-by-Week)
- Nutrition and Long-Term Lifestyle After Bariatric Surgery
- Why Choose Manipal Hospitals Global for Bariatric Surgery?
- Conclusion
What is Bariatric Surgery?
If you are searching what is bariatric surgery, the simplest answer is: it is a medical procedure that helps people lose weight by changing how the stomach and/or intestines work.


Bariatric Surgery Meaning
The bariatric surgery meaning comes from the word “bariatric”, which relates to the treatment of obesity. Bariatric procedures support weight loss by:
- reducing the amount of food the stomach can hold
- changing hunger hormones (such as ghrelin)
- improving insulin sensitivity and blood sugar control
- reducing calorie absorption in certain procedures
- improving long-term satiety and portion control
Bariatric surgery is not cosmetic surgery. It is a metabolic and weight-loss surgery, often recommended when obesity begins affecting overall health and life expectancy.
Who is Eligible for Bariatric Surgery?
Bariatric surgery is usually recommended for patients who have not achieved sustained weight loss through lifestyle changes and medical treatment.
In most international guidelines, bariatric surgery may be advised if:
- BMI ≥ 35 kg/m² (severe obesity), or
- BMI ≥ 30 kg/m² with obesity-related health issues, such as:
- Type 2 diabetes
- High blood pressure
- Obstructive sleep apnoea (OSA)
- Fatty liver disease (NAFLD/NASH)
- Joint pain and mobility limitations
- High cholesterol
- PCOS and infertility issues related to obesity
Some patients with BMI 30–34.9 and uncontrolled diabetes may be considered for metabolic surgery depending on clinical assessment.
Who may not be suitable (or needs optimisation first)?
Your surgeon may postpone or avoid surgery if you have:
- untreated severe depression or active substance misuse
- uncontrolled eating disorders
- very high surgical risk due to heart/lung conditions (though surgery may still be possible with careful planning)
- inability to commit to lifelong dietary changes and follow-ups
Eligibility is decided after a complete medical, nutritional, and psychological evaluation.
Key Benefits of Bariatric Surgery
Many patients assume bariatric surgery is only about weight loss. In reality, the biggest medical advantage is metabolic improvement, especially for diabetes and heart risk.
1) Significant and sustainable weight loss
Most patients lose a meaningful percentage of excess weight over 6–18 months depending on the procedure, lifestyle, and metabolism.
For instance, a person who is 50 kg overweight may typically lose around 35 kg within 12 months.
2) Better control (or remission) of Type 2 diabetes
In many patients, blood sugar levels improve within days to weeks after surgery due to hormonal changes—often even before significant weight loss occurs. Most patients are discharged without any antidiabetic medication and may not require it thereafter.
3) Improvement in blood pressure and cholesterol
Weight reduction and metabolic changes often reduce cardiac risk and the need for long-term medicines.
4) Better sleep and breathing
Patients with obstructive sleep apnoea often see major improvement in snoring, daytime fatigue, and sleep quality.
5) Reduced joint pain and improved mobility
Less body weight reduces pressure on knees, hips, and spine—improving movement and quality of life.
6) Improved fertility and hormonal balance
Many women with obesity-related PCOS experience improved cycle regularity and fertility after weight loss.
7) Better long-term health outcomes
By reducing obesity-related complications, bariatric surgery can lower the risk of future cardiovascular disease and improve life expectancy in medically eligible patients.
Bariatric Surgery Options for International Patients
There are different types of bariatric surgery. Your surgeon chooses the best approach based on your BMI, medical history, eating habits, reflux symptoms, and long-term goals.
1) Sleeve Gastrectomy (Gastric Sleeve)
This procedure removes a large portion of the stomach, leaving a narrow “sleeve.”
How it works:
- Restricts portion size
- Reduces hunger hormones
- Supports steady weight loss
Best suited for:
- patients wanting a simpler procedure than bypass
- patients without severe reflux (or carefully selected reflux cases)
Possible concern: reflux may worsen in some individuals.
2) Roux-en-Y Gastric Bypass (RYGB)
A small stomach pouch is created and connected to a part of the small intestine, bypassing the rest of the stomach and upper intestine.
How it works:
- Restriction + hormonal changes + mild malabsorption
- Very effective for diabetes and reflux control
Best suited for:
- patients with Type 2 diabetes
- patients with significant acid reflux
Considerations: requires long-term vitamin supplementation.
3) Mini Gastric Bypass (One Anastomosis Gastric Bypass)
A simplified form of bypass with one connection, often with shorter operative time.
How it works:
- Similar metabolic benefit as bypass
- Often effective in diabetes and weight loss
Considerations: may cause bile reflux in a small number of patients—careful selection is important.
4) Revision Bariatric Surgery
Some patients who had earlier procedures may require revision due to weight regain, reflux, or complications.
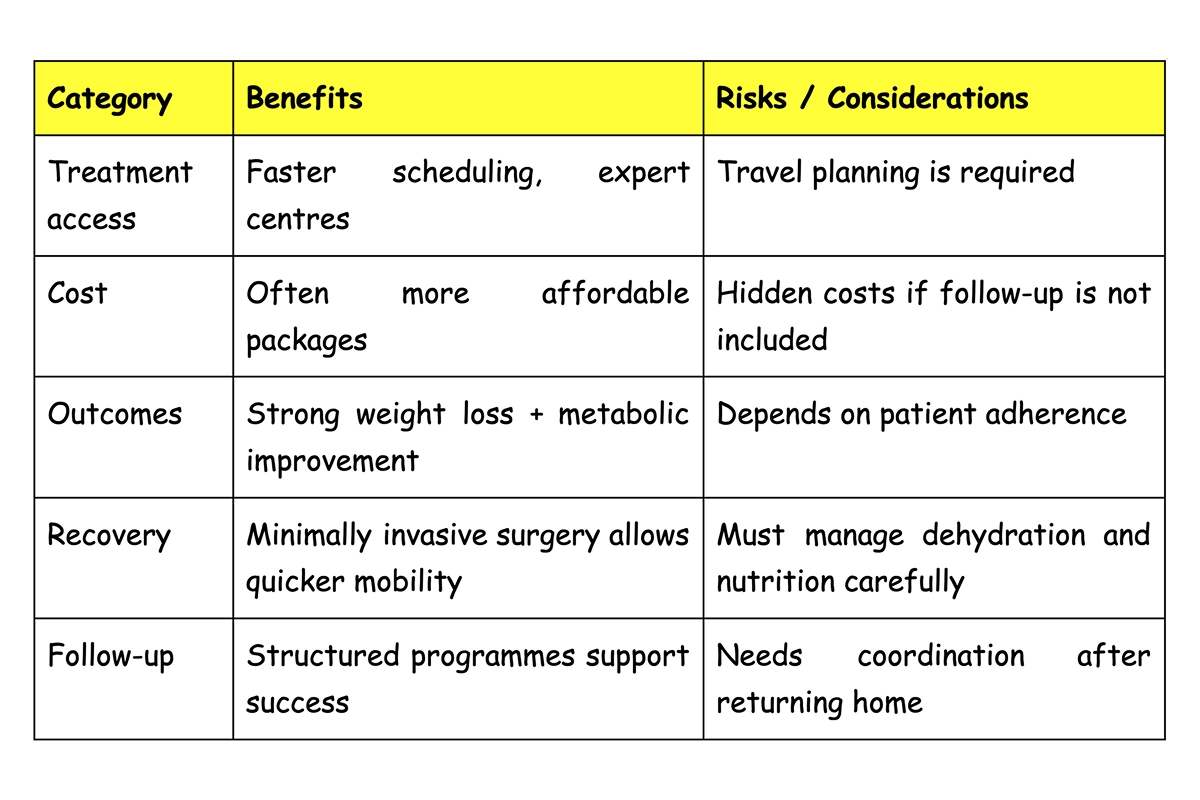
Why Patients Choose Bariatric Surgery Overseas
International patients often travel for bariatric surgery because of:
- access to experienced surgeons with high case volumes
- modern laparoscopic and minimally invasive techniques
- shorter waiting time compared to certain countries
- high-quality hospital infrastructure (ICU, multidisciplinary teams)
- bundled packages covering surgery, stay, investigations, and follow-ups
- support teams for travel, language, and care coordination
That said, the best outcomes come when overseas surgery is planned like a medical journey, not a rushed trip.
Bariatric Surgery Cost: What International Patients Should Know
The bariatric surgery cost varies widely based on:
- country and hospital accreditation
- surgeon expertise
- procedure type (sleeve vs bypass vs revision)
- length of hospital stay
- ICU requirement (if any)
- pre-operative tests and specialist consultations
- post-operative diet counselling and follow-up plans
A helpful way to think about total cost
Instead of focusing only on surgery fees, consider the complete cost of safe treatment, including:
- pre-surgery evaluation (blood work, scans, cardiac clearance)
- anaesthesia and OT charges
- hospital stay (usually 2–4 days)
- medications, compression stockings, and DVT prevention
- dietician guidance and discharge planning
- follow-up coordination after you return home
Low-cost quotes that do not include essential safety steps may increase complication risk.
Risks of Bariatric Surgery (Realistic and Medically Accurate)
Bariatric surgery is considered safe when performed in a well-equipped centre by trained teams, but it is still major surgery. Understanding risks helps you plan responsibly.
Common short-term risks (first few days to weeks)
- bleeding
- infection
- nausea or vomiting
- blood clots (DVT/PE) without proper prevention
- leak from the staple line or surgical join (rare but serious)
Medium-term risks (weeks to months)
- gallstones due to rapid weight loss
- dumping syndrome (more common in bypass)
- constipation
- hair thinning (usually temporary, linked to low protein intake)
Long-term risks
- vitamin and mineral deficiencies (iron, B12, calcium, vitamin D)
- low protein intake causing fatigue and muscle loss
- weight regain if lifestyle changes are not followed
- narrowing/stricture (rare)
- ulcers (especially with smoking or NSAID use after bypass)
Important: Most complications can be reduced with proper surgeon selection, hospital protocols, and structured follow-ups.
Preparing for Bariatric Surgery Hospital Admission, Surgery & Discharge Flow
Hospital Admission, Surgery & Discharge Flow
- After completing all required investigations—including blood tests and fitness evaluations—the patient is admitted either a day prior to surgery or on the day of surgery itself.
- Bariatric surgery is usually performed laparoscopically and typically takes 1–2 hours, depending on the procedure and patient factors.
- A few hours after surgery, patients are encouraged to start walking, which helps reduce the risk of blood clots and supports faster recovery.
- Oral fluids are usually started the next day, under medical supervision.
- Most patients are discharged on Day 2 after surgery, once pain is controlled, fluids are tolerated, and mobility is comfortable.
- For the majority of patients, ICU stay is not required, as recovery is smooth with standard post-operative monitoring.
Step 1: Share complete medical history early
Include:
- diabetes and current medications
- heart history
- sleep apnoea details
- thyroid profile
- previous abdominal surgeries
- current weight trends and diet history
Step 2: Pre-operative evaluation
Most bariatric centres will recommend:
- CBC, kidney/liver profile
- blood sugar (HbA1c), lipid profile
- thyroid tests
- ECG and chest X-ray
- ultrasound abdomen (fatty liver/gallbladder)
- cardiac clearance (if needed)
- sleep assessment if OSA suspected
Step 3: Pre-surgery weight loss diet
Many surgeons recommend a liver-shrinking diet for 1–2 weeks pre-op to improve surgical safety and visibility during laparoscopy.
Step 4: Plan your stay duration abroad
For most international patients, it is wise to plan:
- 7–14 days total stay depending on surgery type, recovery, and travel tolerance.
Step 5: Prepare your post-surgery support system
You should know:
- who will help you during recovery at home
- where you will get follow-up blood tests
- who to contact in case of complications
Bariatric Surgery Recovery Timeline (Week-by-Week)
Recovery is not just “healing of stitches.” It includes rebuilding strength, adjusting nutrition, preventing dehydration, and learning new eating behaviour.
Hospital Stay (Day 0 to Day 3/4)
What happens:
- surgery is usually done laparoscopically
- walking begins within 6–12 hours
- pain is managed with medicines
- you start sipping fluids as advised
Discharge is planned when:
- you can drink fluids without vomiting
- pain is controlled
- vitals and labs are stable
- you can walk comfortably
Week 1: The Hydration Week
Focus:
- sipping small amounts every few minutes
- avoiding dehydration (dry mouth, dizziness, dark urine)
- managing nausea early
Diet: clear liquids → full liquids (as per surgeon)
Activity: gentle walking every few hours
Week 2: Transition to thicker fluids
Diet:
- protein shakes
- soups (strained)
- yoghurt / smooth liquids (as advised)
Common symptoms:
- tiredness
- mild abdominal discomfort
- constipation due to low intake
Many patients feel better but still have low energy.
Weeks 3–4: Soft foods begin
Diet: soft, mashed foods in very small portions
- eggs (if tolerated)
- soft cooked vegetables
- minced lean proteins
- paneer/tofu
- mashed lentils in controlled quantity
Focus:
- protein first
- chew slowly
- stop at fullness (even if it feels “too little”)
Overeating can cause vomiting or pain.
Weeks 5–6: Normal textured foods start gradually
Your stomach will still be healing internally, so portions remain small.
You may return to work (depending on job type):
- desk job: around 2–3 weeks (sometimes earlier)
- physically demanding job: 4–6 weeks
Months 2–3: Visible weight loss phase
You will notice:
- consistent weight loss
- improved sugar levels and blood pressure
- better sleep
- improved movement
Important check: blood tests may be planned to monitor nutrient levels.
Months 6–12: Stabilisation and lifestyle mastery
This phase defines long-term results.
Best habits for success:
- prioritise protein daily
- strength training to prevent muscle loss
- avoid liquid calories and sugary drinks
- keep follow-ups and nutrition monitoring
Nutrition and Long-Term Lifestyle After Bariatric Surgery
Bariatric surgery is a tool—not a cure by itself. Long-term success depends heavily on consistent habits.
Protein matters
Protein prevents:
- weakness
- hair fall
- muscle loss
- slow recovery
Vitamins are lifelong (especially after bypass)
Most patients need some combination of:
- multivitamin
- calcium + vitamin D
- vitamin B12
- iron (especially women)
Your surgeon decides based on procedure and lab results.
Hydration and portion discipline
Small stomach capacity means you must drink regularly but avoid drinking too fast. Also, you may need to avoid drinking immediately with meals (as advised).
Why Choose Manipal Hospitals Global for Bariatric Surgery?
For international patients, choosing the right hospital is not only about surgery success—it’s about safety, coordination, and recovery support.
At Manipal Hospitals Global, bariatric surgery care is supported by:
- experienced bariatric and GI surgeons
- advanced laparoscopic OT infrastructure
- multidisciplinary evaluation (medicine, anaesthesia, dietetics)
- structured post-operative nutrition progression
- safety protocols for clot prevention and early mobilisation
- international patient support for scheduling and continuity of care
A well-planned bariatric programme improves outcomes, reduces complications, and helps patients return home confidently with a long-term roadmap.
Conclusion
Planning bariatric surgery overseas can be a smart and effective decision when done responsibly. The best outcomes come from choosing a reputable hospital, completing proper pre-surgery assessments, understanding the realistic risks, and committing to long-term follow-up.
If you are considering bariatric surgery, remember that the procedure is only the start of your transformation. With the right medical team, nutrition planning, and lifestyle support, bariatric surgery can improve not only weight—but also diabetes control, heart health, mobility, confidence, and overall quality of life.
Share this Article


Not sure what you’re looking for?
Not sure what you’re looking for?
Get in touch with our representatives for
help!
Get in touch with our
representatives for help!

