Digestive Disorders: Symptoms, Diagnosis, and Treatment Options for International Patients
Reviewed by: Gastro Science Department
Posted on Mar 02, 2026
6 Min Read

When digestive problems keep coming back, no matter what you try, where do you go from there? Living with digestive disorders can be physically draining and emotionally exhausting. When symptoms linger despite medication, or when specialised procedures are not easily available locally, the thought of seeking care overseas naturally begins to surface. For many patients, travelling for digestive disorder treatment is not simply about convenience. It is about access to advanced diagnostics, experienced multidisciplinary teams, and timely intervention before complications arise. The decision, however, brings its questions: Is it safe? What tests will be required? How long will recovery take?
This blog explores digestive disorders in depth while guiding international patients through the practical and medical realities of seeking treatment overseas. From recognising symptoms and understanding complex digestive system disorders to evaluating modern treatment options and planning cross-border care, you will find clear, structured insights to help you make informed decisions with confidence.
Synopsis
- What Are Digestive Disorders?
- Common Symptoms You Should Not Ignore
- Major Types of Digestive System Disorders
- Why Patients Often Seek Treatment Overseas
- How Digestive Disorders are Diagnosed
- Treatment Options for Digestive Disorders
- Specialised Procedures for Treating Digestive Disorders
- Preparing for Treatment Abroad
- Long-Term Outlook and Monitoring
- Conclusion
What Are Digestive Disorders?
The digestive system is a long, coordinated pathway that begins at the mouth and ends at the rectum. It is responsible for breaking down food, absorbing nutrients, and eliminating waste. When any part of this system malfunctions, symptoms can range from mild discomfort to life-altering complications.
Digestive disorders refer to conditions affecting the oesophagus, stomach, small intestine, large intestine, liver, pancreas, or gallbladder. Some are short-term and manageable. Others are chronic and require structured medical care. While digestive system disorders vary widely in cause and severity, they all share one common factor: they interfere with the body’s ability to process food efficiently and safely.
Common Symptoms You Should Not Ignore
Digestive symptoms are often subtle at first. However, certain patterns deserve medical attention, particularly if they persist for more than a few weeks or gradually worsen.
Some warning signs include:
● Persistent abdominal pain or cramping
● Frequent bloating or excessive gas
● Ongoing diarrhoea or constipation
● Blood in stool or black, tarry stools
● Difficulty swallowing
● Unexplained weight loss
● Recurrent nausea or vomiting
● Chronic acid reflux or heartburn
Occasional discomfort after a heavy meal is common. But repeated symptoms may indicate underlying digestive system disorders such as inflammatory bowel disease, peptic ulcer disease, coeliac disease, or chronic pancreatitis. Early evaluation reduces the risk of complications and improves long-term outcomes.
Major Types of Digestive System Disorders
Digestive disorders are not a single disease. They include a broad spectrum of conditions, each with distinct causes and treatment pathways. Understanding the category your symptoms fall into helps guide the next steps.
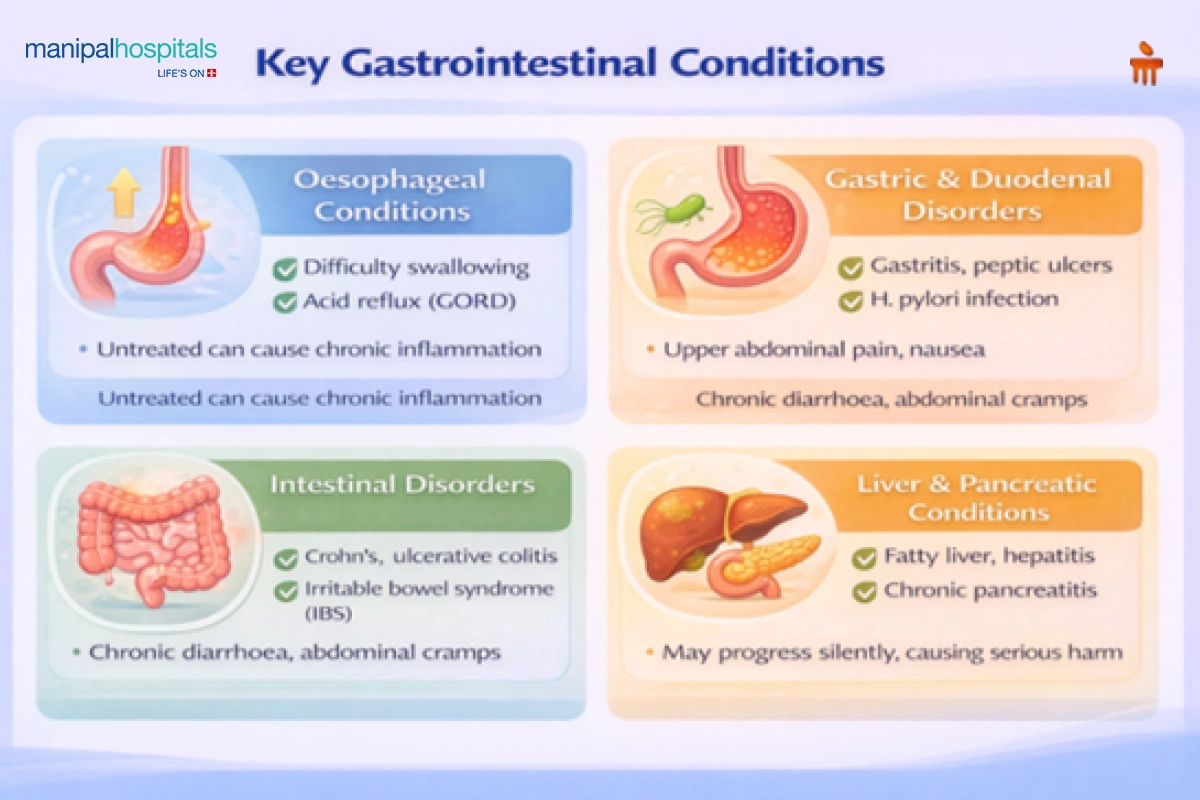
1. Oesophageal Conditions
These involve difficulty swallowing, chest discomfort, or acid reflux. Conditions such as gastro-oesophageal reflux disease (GORD) can lead to chronic inflammation if untreated.
2. Gastric and Duodenal Disorders
These include gastritis and peptic ulcers, often linked to Helicobacter pylori infection or prolonged use of certain medications. Symptoms may include upper abdominal pain and nausea.
3. Intestinal Disorders
Inflammatory bowel diseases like Crohn’s disease and ulcerative colitis are chronic autoimmune conditions affecting the intestines. Irritable bowel syndrome, although functional rather than inflammatory, can significantly impact daily life.
4. Liver and Pancreatic Conditions
Fatty liver disease, hepatitis, and chronic pancreatitis fall into this category. These may initially present with vague symptoms but can progress silently if ignored.
Each digestive disorder has unique risk factors, progression patterns, and management strategies. Accurate classification is crucial before starting any digestive disorder treatment.
Why Patients Often Seek Treatment Overseas
Patients often travel abroad for advanced care when local options are limited, waiting times are long, or specialised expertise is unavailable. Digestive disorders sometimes require multidisciplinary evaluation involving gastroenterologists, hepatologists, surgeons, nutritionists, and interventional radiologists.
International centres frequently offer:
● Advanced endoscopic procedures
● High-resolution imaging
● Minimally invasive surgery
● Comprehensive nutritional rehabilitation
● Coordinated follow-up plans
For chronic digestive system disorders and treatments that require long-term monitoring, structured international programmes can provide continuity and clarity.
How Digestive Disorders are Diagnosed
Diagnosis begins with a detailed medical history. Patterns matter: when symptoms occur, what triggers them, how long they last, and whether there is a family history of gastrointestinal disease.
Doctors may recommend investigations such as:
● Blood tests to detect inflammation, anaemia, or liver dysfunction
● Stool tests to identify infection or hidden blood
● Endoscopy to directly visualise the oesophagus, stomach, or colon
● Imaging scans such as CT or MRI
● Biopsy to confirm inflammatory or malignant changes
Accurate diagnosis prevents unnecessary treatments. A structured evaluation also helps international patients plan their travel efficiently, often completing tests within a coordinated timeframe.
Treatment Options for Digestive Disorders
Management depends entirely on the diagnosis. There is no single universal digestive disorder treatment. Instead, therapy is tailored to the underlying cause, severity, and patient-specific factors.
Medical Management
For many digestive disorders, medication forms the foundation of treatment. These may include:
● Acid-suppressing medicines for reflux
● Anti-inflammatory drugs for inflammatory bowel disease
● Antibiotics for bacterial infections
● Enzyme supplements for pancreatic insufficiency
● Immunomodulators for autoimmune conditions
Medication plans are carefully monitored to prevent side effects and ensure sustained benefit.
Endoscopic Procedures
Advances in therapeutic endoscopy have reduced the need for open surgery in many cases. Doctors can now remove polyps, dilate strictures, control bleeding, and treat early tumours using minimally invasive techniques. Recovery is typically faster compared to traditional surgery.
Surgical Intervention
Surgery becomes necessary when complications arise or when medical therapy fails. This may include bowel resection for severe inflammatory disease, gallbladder removal for gallstones, or liver surgery in selected cases.
Nutritional and Lifestyle Therapy
Nutrition plays a central role in digestive system disorders and treatments. A personalised dietary plan can reduce symptom flare-ups and prevent malnutrition. Lifestyle modifications such as structured meal timing, reduced alcohol intake, and stress management significantly improve outcomes.
Specialised Procedures for Treating Digestive Disorders
Procedure | Primary Indication | Average Hospital Stay | Recovery Timeline | Special Considerations |
Endoscopic Submucosal Dissection (ESD) | Early gastrointestinal tumours | 1-2 days | 1-2 weeks | Requires high operator expertise |
ERCP (Endoscopic Retrograde Cholangiopancreatography) | Bile duct stones or obstruction | Same day or overnight | Few days | Risk of pancreatitis, monitored closely |
Laparoscopic Colectomy | Complicated colitis or tumours | 4-6 days | 4-6 weeks | Minimally invasive, smaller scars |
Liver Transplant Evaluation Programme | End-stage liver disease | Variable | Long-term follow-up required | Multidisciplinary assessment essential |
Capsule Endoscopy | Small bowel bleeding or obscure symptoms | Outpatient | Immediate return to normal activity | Non-invasive diagnostic tool |
Preparing for Treatment Abroad
Travelling for healthcare requires careful planning. International patients should gather previous medical records, imaging reports, biopsy results, and medication lists before consultation.
It is also important to:
● Discuss travel safety if experiencing severe symptoms
● Confirm post-treatment follow-up plans
● Understand medication availability in your home country
● Arrange accommodation close to the treating facility
Clear communication between the treating team and local doctors ensures continuity of care after returning home.
Long-Term Outlook and Monitoring
Many digestive disorders are chronic conditions requiring ongoing monitoring. Remission is possible in several inflammatory conditions, while others need lifelong lifestyle adjustments.
Regular follow-up prevents complications such as intestinal narrowing, nutritional deficiencies, or progression of liver disease. Early detection of recurrence allows timely intervention. With structured care, most patients achieve symptom control and a stable quality of life.
For individuals considering digestive disorder treatment abroad, especially in centres offering advanced care in metropolitan hubs such as London, comprehensive programmes for digestive system disorders and treatments can provide coordinated and evidence-based management under specialist supervision.
Conclusion
Digestive symptoms should never be brushed aside as minor inconveniences. Persistent discomfort, altered bowel habits, or unexplained weight changes may signal underlying digestive disorders that require structured medical evaluation.
With accurate diagnosis, tailored digestive disorder treatment, and multidisciplinary expertise, outcomes have improved significantly over the past decade. At Manipal Hospitals Global, international patients get access to advanced diagnostics, minimally invasive procedures, and long-term management strategies that address both immediate symptoms and future risk. Seeking timely care improves recovery and restores confidence in your health journey.
Share this Article


Not sure what you’re looking for?
Not sure what you’re looking for?
Get in touch with our representatives for
help!
Get in touch with our
representatives for help!

